Finding a rash on your baby’s skin can be terrifying. You see a red bump and your mind immediately jumps to the worst-case scenario. We have been there.
The good news? Most baby rashes are completely harmless and clear up on their own within a few days. However, it is always smart to keep a close watch on any skin changes.
Our medical team has broken down the 17 most common types of baby rashes. We will help you identify those bumps so you can stop worrying and start treating them correctly.
Key Takeaways
- Check the symptoms: Examine the rash for color, texture (blisters vs. flat patches), and location to narrow down the cause.
- Watch behavior: If your baby has a fever, is lethargic, or seems in pain, these are signs the rash might need medical attention.
- Ask a pro: When in doubt, call your pediatrician. It is always better to be safe, especially with rapid skin changes.
- Prevention helps: Keep skin clean, dry, and moisturized. Avoid harsh detergents and known allergens to stop rashes before they start.
- 1. Baby Acne
- 2. Cradle Cap
- 3. Erythema Toxicum Neonatorum (ETN)
- 4. Atopic Eczema
- 5. Hives
- 6. Diaper Rash
- 7. Milia
- 8. Impetigo
- 9. Fifth Disease
- 10. Hand, Foot, and Mouth Disease
- 11. Measles
- 12. Miliaria (Heat Rash)
- 13. Scabies
- 14. Ringworm
- 15. Meningitis
- 16. Chickenpox
- 17. Molluscum Contagiosum
- When to Worry
- Rashes FAQs
- Rash Decision
1. Baby Acne
Don’t panic if your newborn looks like a tiny teenager. Baby acne is incredibly common. It usually pops up within the first two weeks of life and can hang around for a few days or even months (1).
Causes
Doctors aren’t 100% sure why this happens, but the leading theory is maternal hormones. Your baby is exposed to your hormones in the womb, which can stimulate their oil glands after birth.
Symptoms
Baby acne looks just like the adult version. Expect tiny red or white pimples on the cheeks, nose, forehead, and chin.
Treatment
The best treatment is often no treatment at all. Keep the area clean by gently wiping it with water and a soft cloth.
You can use a mild baby lotion, but don’t overdo it. Clogging the pores can make things worse. Avoid teenage acne creams or harsh scrubs; newborn skin is far too delicate for those chemicals.
If the acne looks infected or doesn’t clear up after a few months, check in with your pediatrician. It is rarely a sign of a hormonal issue, but it is worth ruling out.
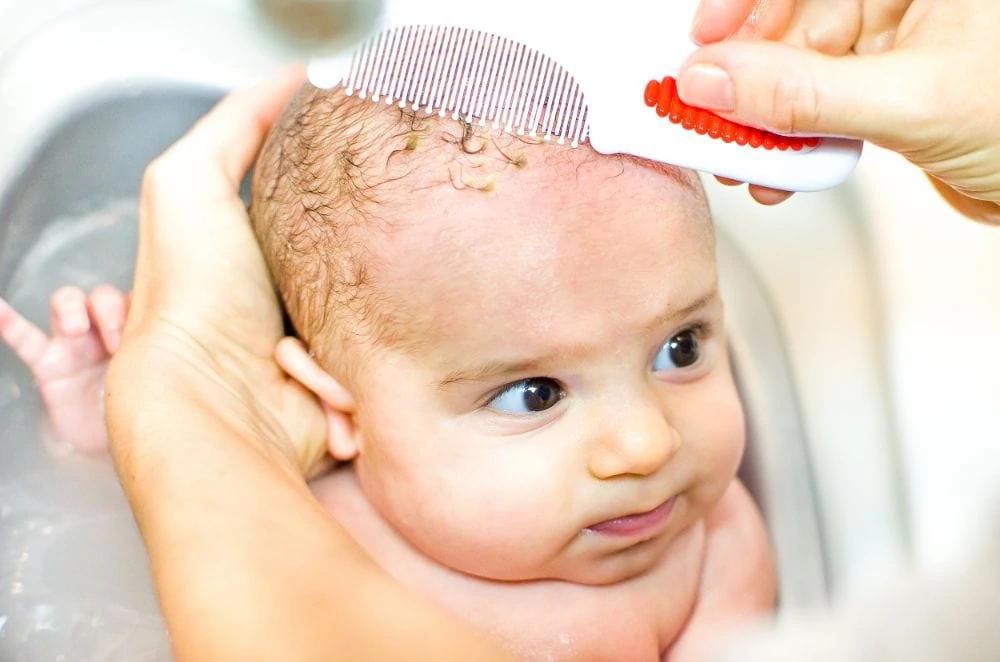
2. Cradle Cap
Cradle cap is the infant version of dandruff. It looks like greasy yellow or brown scales on the scalp. It usually appears in the first few months and is not contagious (2).
Causes
While the exact cause is a mystery, two factors likely play a role:
- Fungus: A yeast called Malassezia, which lives on skin naturally, might grow out of control.
- Sebum: Your baby’s glands might produce too much oil, trapping skin cells.
Symptoms
It looks worse than it feels. Your baby likely won’t be bothered by it. You will see crusty patches on the head that might flake off, sometimes taking a little hair with them. In severe cases, it can smell a bit oily.
Treatment
It often resolves on its own, but you can speed things up with a simple routine:
- Wash and brush: Use a mild shampoo and gently brush the scalp with a soft bristle brush to loosen scales.
- Oil treatment: Massage baby oil or coconut oil onto the scalp before a bath to soften the crust.
- Special shampoos: For stubborn cases, cradle cap shampoos can help break down the scales.
Whatever you do, don’t pick the scales with your fingernails. This can cause small wounds and lead to infection.
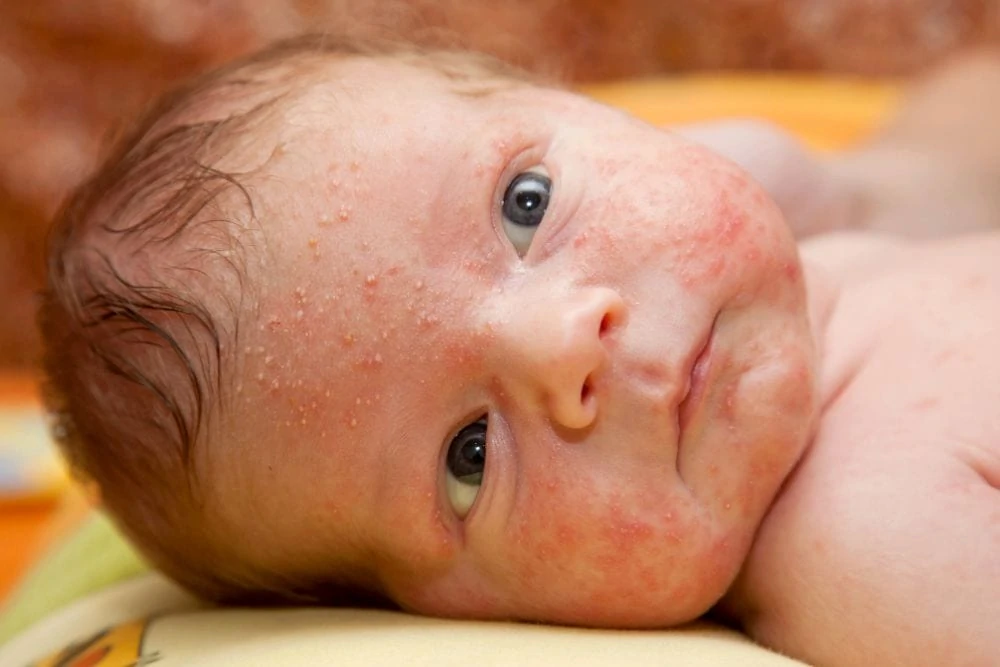
3. Erythema Toxicum Neonatorum (ETN)
The name sounds scary, but ETN is very common and harmless. It appears in the first few days of life, mostly in full-term babies (3).
Causes
The cause is unknown. Experts believe it is just the baby’s immune system waking up and adjusting to life outside the womb.
Symptoms
ETN looks like blotchy red spots, often with a small white or yellow bump in the center. It can look like a flea bite. It usually appears on the chest, face, and back but spares the palms and soles of the feet.
Treatment
No treatment is needed. It disappears on its own within a week. If the bumps contain pus or your baby seems unwell, call your doctor to rule out infection.
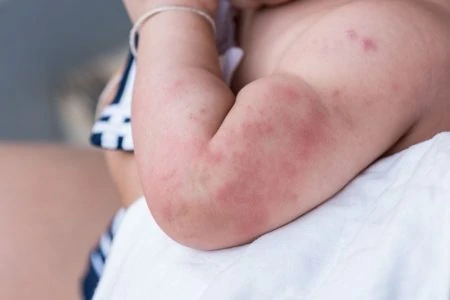
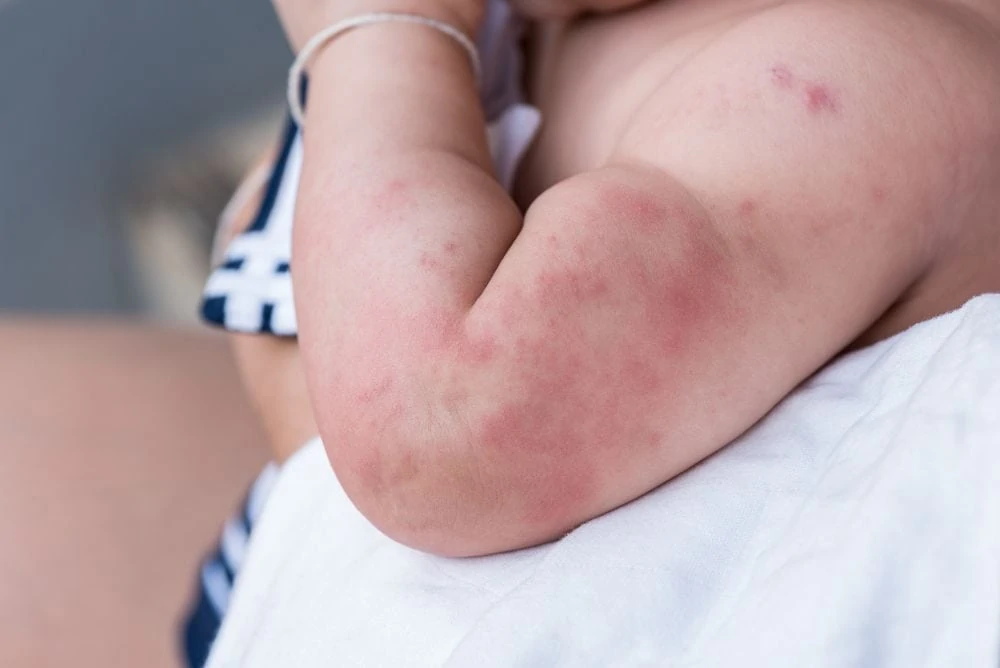
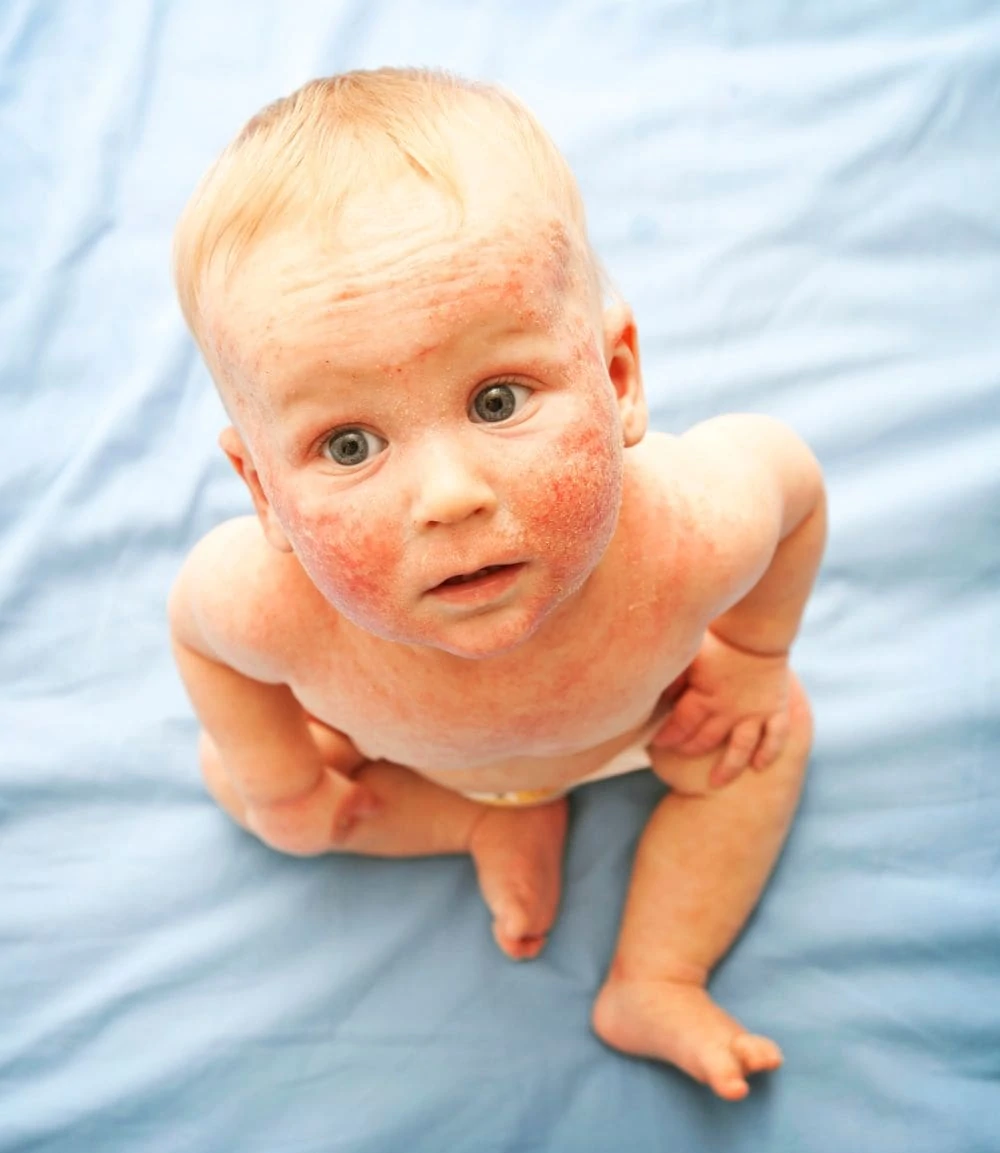
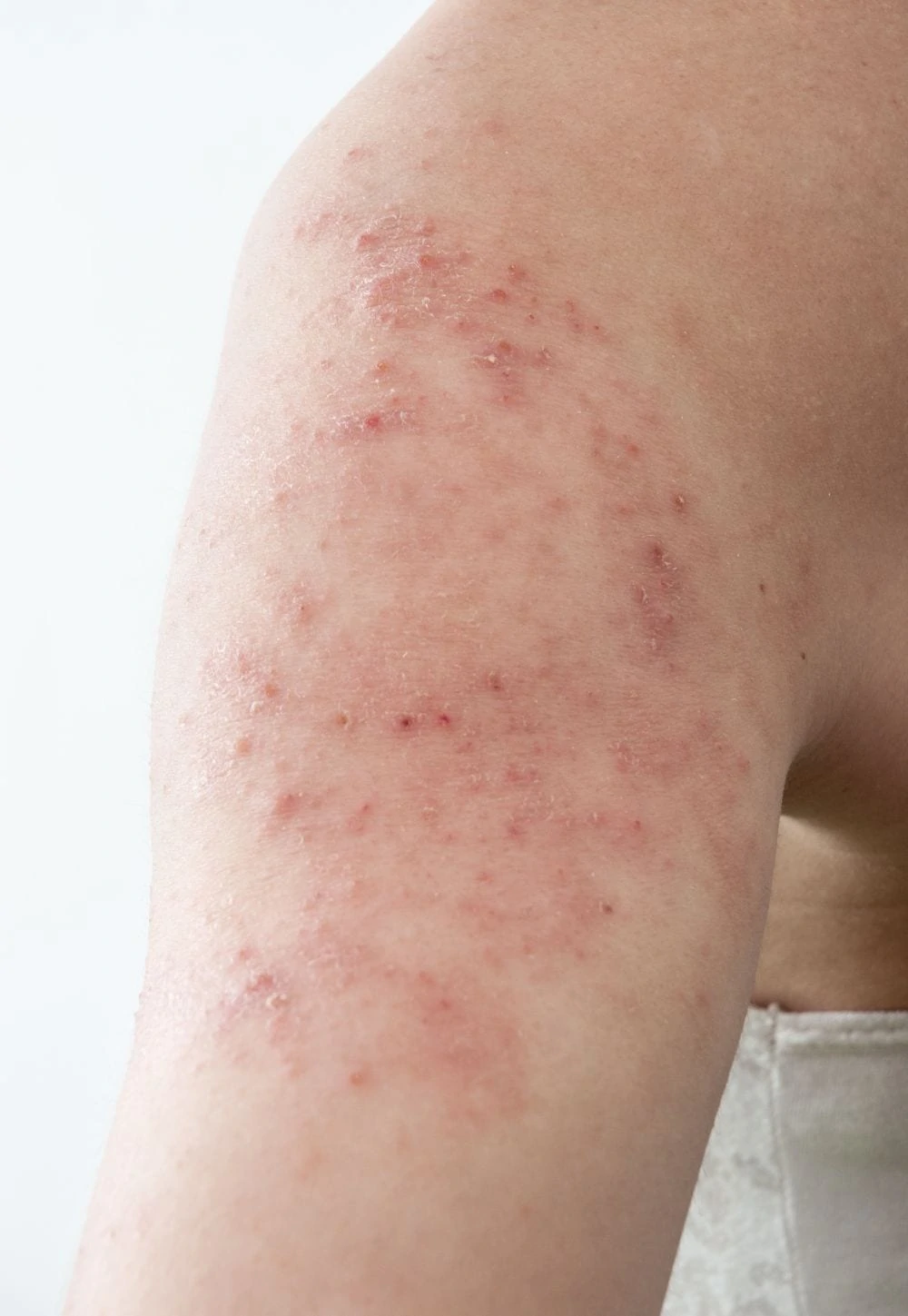
4. Atopic Eczema
Eczema is a chronic condition that makes skin red, itchy, and dry. It can be uncomfortable for babies, leading to fussiness (4).
Causes
Genetics play a huge role. If you or your partner have eczema, asthma, or hay fever, your baby is more likely to have it. Triggers include:
- Irritants: Scented soaps, laundry detergents, and bubble baths.
- Environment: Cold dry air, heat, and sweat.
- Allergens: Dust mites, pet dander, or certain foods.
Symptoms
Look for dry, scaly patches that turn red and inflamed. On babies, it often starts on the cheeks or scalp, then spreads to the elbows and knees. It is incredibly itchy.
Treatment
Hydration is key. Use thick, fragrance-free eczema creams or ointments immediately after baths to lock in moisture.
Identify and remove triggers. Switch to sensitive skin detergents and avoid wool clothing. If the rash is severe, your pediatrician might prescribe a mild steroid cream. Scratch mittens can also prevent your baby from breaking the skin and causing an infection.
5. Hives
Hives are raised, red itchy welts that can appear anywhere. They often show up suddenly and move around the body (5).
Causes
Hives are an immune response. The body releases histamine, causing swelling. Common triggers include:
- Viral infections: Surprisingly, colds and viruses are a very common cause of hives in kids.
- Allergens: Foods (like eggs or nuts), medications, insect bites, or pet dander.
- Temperature: Extreme cold or heat.
Symptoms
The rash looks like mosquito bites or large red blotches with pale centers. They can range from tiny spots to large plates. A key sign is that they “blanch” (turn white) when you press them.
Treatment
If your baby is comfortable, you can wait it out. Cool compresses or a lukewarm bath can help the itch.
For significant discomfort, your doctor might suggest an antihistamine like Benadryl. **Important:** If hives are accompanied by wheezing, vomiting, or swelling of the lips/tongue, call 911 immediately. This could be anaphylaxis.
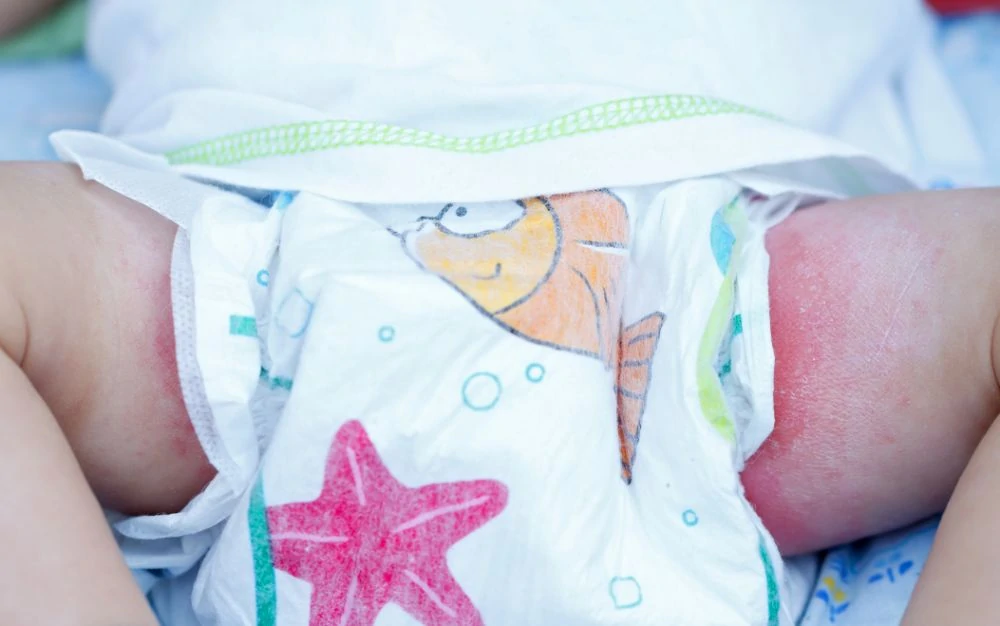
6. Diaper Rash
Diaper rash is practically a rite of passage. It is caused by moisture and irritation in the diaper area (6).
Causes
The main culprits are:
- Moisture: Sitting in a wet or dirty diaper for too long.
- Chafing: Diapers that are too tight.
- New foods: Acidic foods (like tomatoes or strawberries) can change the stool composition.
- Yeast: A bright red rash in the skin folds is often a fungal infection.
Symptoms
The skin on the glutes, thighs, and genitals looks red and tender. Your baby may cry during diaper changes.
Treatment
The golden rule is to keep it clean and dry. Change diapers frequently. Use a thick barrier cream containing zinc oxide to protect the skin from moisture.
Give your baby some “air time” without a diaper to let the skin breathe. If you use cloth diapers, ensure you are using a residue-free detergent.
7. Milia
Milia, often called “milk spots,” are tiny white bumps that usually appear on a newborn’s face (7).
Causes
Dead skin flakes become trapped in small pockets near the surface of the skin. It is completely normal and not related to breastfeeding.
Symptoms
You will see pearl-white bumps on the nose, cheeks, or chin. They can also appear on the gums (called Epstein pearls). They don’t itch or hurt.
Treatment
Do nothing. Seriously. Milia will disappear on their own within a few weeks as the skin pores open up. Never squeeze them, or you risk scarring your baby’s face.
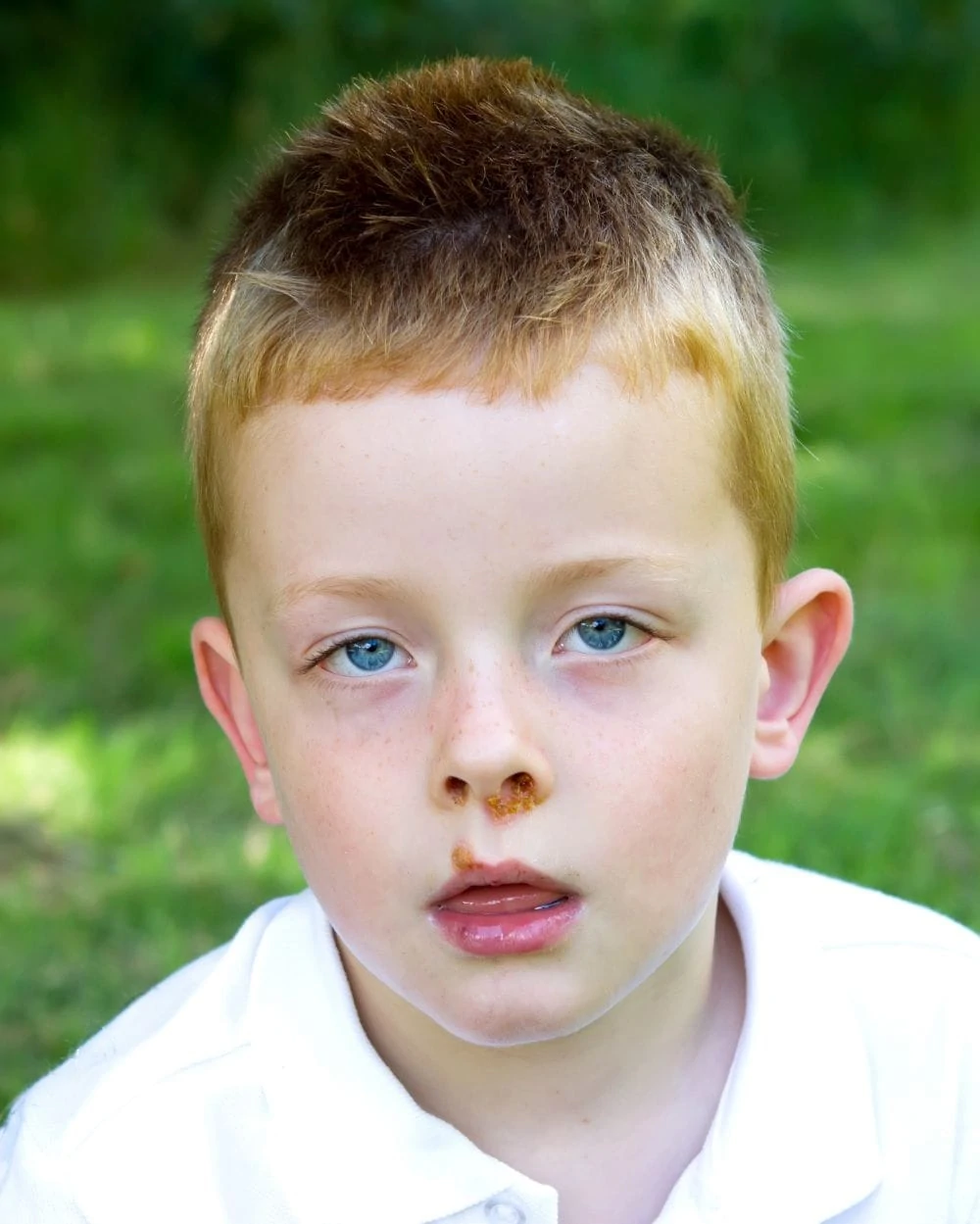
8. Impetigo
Impetigo is a bacterial infection often called “school sores,” though babies can get it too. It is highly contagious (8).
Causes
Bacteria (staph or strep) get into the skin through a small cut, scratch, or bug bite. It spreads easily through touch or shared towels.
Symptoms
Look for red sores that burst and form a honey-colored crust. It is common around the nose and mouth but can spread to hands and diaper areas. It can be itchy and painful.
Treatment
You need to see a doctor for this one. They will likely prescribe a topical antibiotic ointment or oral antibiotics for widespread cases.
Keep the sores clean and trim your baby’s nails to prevent scratching and spreading the bacteria. Wash sheets and towels daily in hot water until the infection clears.
9. Fifth Disease
Also known as “slapped cheek syndrome,” this viral illness is famous for the bright red rash it causes on the face (9).
Causes
It is caused by parvovirus B19. It spreads through respiratory droplets (coughs and sneezes). Once the rash appears, the child is usually no longer contagious.
Symptoms
It often starts with mild cold symptoms like a runny nose and low fever. A few days later, bright red cheeks appear. A lacy, pink rash may also spread to the arms, legs, and trunk.
Treatment
Since it is a virus, antibiotics won’t work. It usually clears up on its own in a week or two. Keep your child comfortable with fluids and rest.
**Note for Moms:** If you are pregnant and exposed to Fifth disease, contact your OB-GYN, as it can occasionally cause complications for the fetus.
10. Hand, Foot, and Mouth Disease
This virus is notorious in daycares. As the name suggests, it causes spots on the hands, feet, and inside the mouth (10).
Causes
It is caused by the coxsackievirus. It spreads through saliva, mucus, and stool (dirty diapers). It is extremely contagious.
Symptoms
Symptoms include:
- Fever and sore throat.
- Painful sores in the mouth (herpangina) that can make eating difficult.
- Red spots or blisters on palms, soles, and sometimes the buttocks.
A few weeks later, fingernails or toenails may peel off. Don’t worry; they grow back!
Treatment
There is no specific cure. Manage the fever and pain with acetaminophen or ibuprofen (if the baby is old enough). Cold foods like popsicles or ice cream can numb the mouth sores. Keep them hydrated!
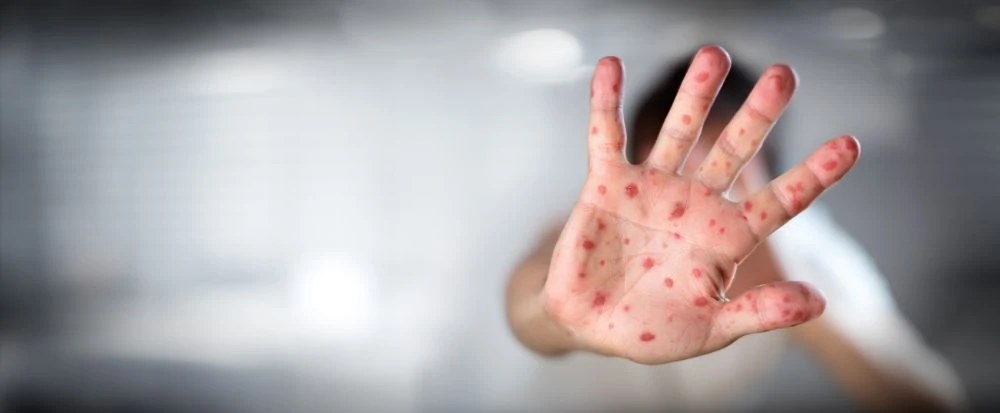
11. Measles
Measles is a serious viral infection that used to be common but is now preventable with vaccines. However, outbreaks still occur (11).
Causes
It is caused by the measles virus, which is airborne. If an infected person coughs in a room, the virus can linger in the air for up to two hours. It is one of the most contagious diseases on earth.
Symptoms
It starts with a high fever, cough, runny nose, and red, watery eyes. Tiny white spots (Koplik spots) may appear inside the mouth.
A few days later, a flat red rash begins at the hairline and spreads downward to the neck, trunk, and limbs.
Treatment
Call your doctor immediately if you suspect measles. Do not go directly to the waiting room, as you could infect other babies.
Treatment is supportive: rest, fluids, and fever reducers. Vitamin A supplements can sometimes help reduce severity. The best protection is the MMR vaccine, given at 12, 15 months.
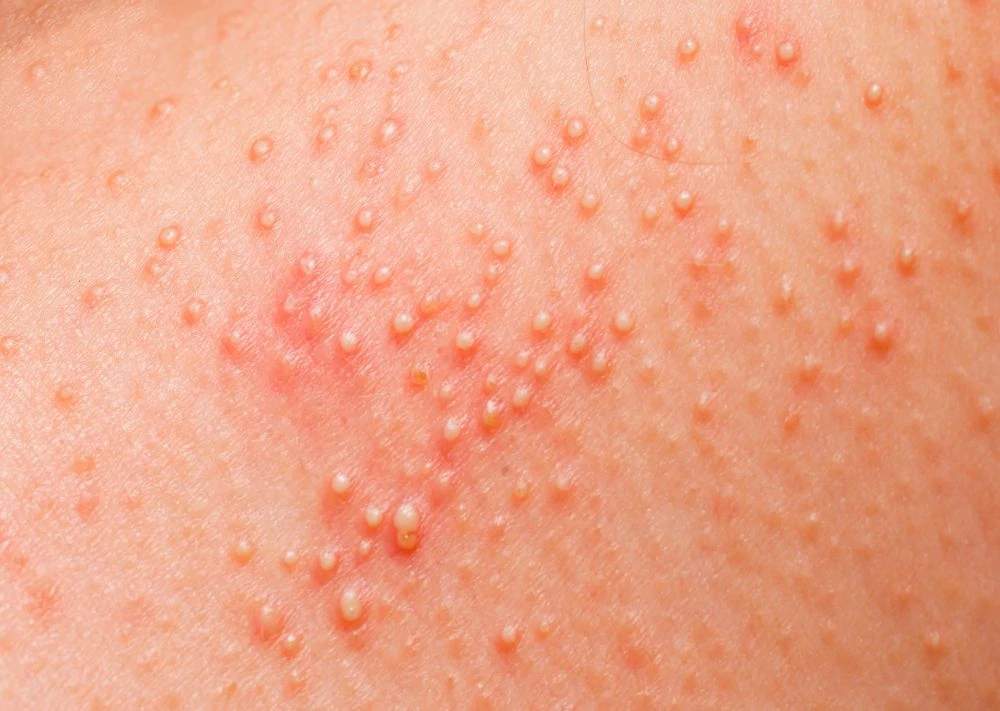
12. Miliaria (Heat Rash)
Also known as heat rash or prickly heat, this happens when your baby gets too hot (12).
Causes
Babies have tiny sweat ducts that clog easily. If they are dressed too warmly or the weather is humid, sweat gets trapped under the skin.
Symptoms
You will see clusters of small red bumps or tiny clear blisters. It usually appears in skin folds, on the neck, or upper chest. It can cause a “prickly” stinging sensation.
Treatment
Cool the baby down. Remove heavy clothing and move to a cooler room or use a fan. The rash usually fades quickly once the skin cools. Avoid heavy creams, which can block pores further.
13. Scabies
Scabies is an intensely itchy skin infestation. It is not about hygiene; anyone can get it (13).
Causes
Microscopic mites burrow into the top layer of skin to lay eggs. It spreads through prolonged skin-to-skin contact.
Symptoms
The main symptom is severe itching, which is usually worse at night. You might see small, red bumps or wavy lines (burrows) on the skin, often between fingers, on wrists, or in armpits.
Treatment
You need a prescription cream (usually Permethrin) to kill the mites. **Crucial:** Everyone in the household must be treated at the same time, even if they don’t have symptoms, or the mites will just pass back and forth. Wash all bedding and clothes in hot water.
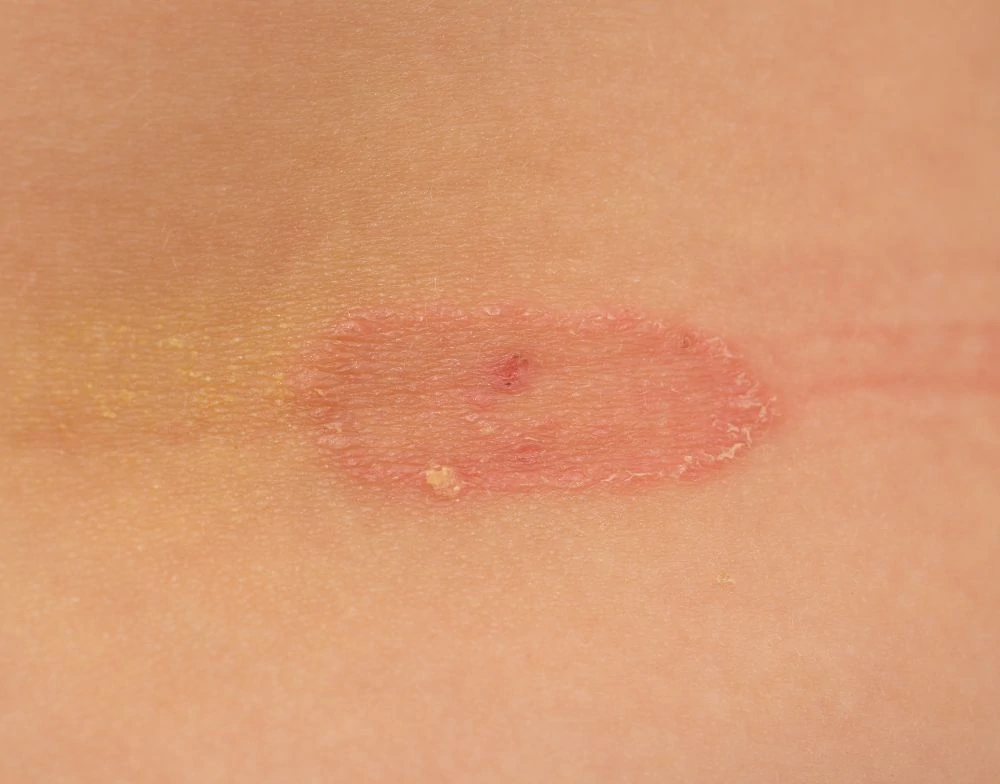
14. Ringworm
Despite the name, there are no worms involved! Ringworm is a common fungal infection (14).
Causes
A fungus (tinea) causes it. It thrives on warm, moist skin and spreads via contact with infected people, pets (check your dog or cat!), or contaminated surfaces like sheets.
Symptoms
It looks like a red, scaly ring with a clear center. The border is slightly raised and can be itchy. On the scalp, it can cause round patches of hair loss.
Treatment
Over-the-counter antifungal creams (like clotrimazole) usually work well. Apply it for the full duration recommended, even if the rash looks better. If it is on the scalp, you will likely need a prescription oral medication.
15. Meningitis
Meningitis is a rare but life-threatening infection of the membranes covering the brain and spinal cord. It requires immediate emergency care (15).
Causes
It can be viral or bacterial. Bacterial meningitis is the most dangerous and can lead to sepsis (blood poisoning).
Symptoms
The classic sign is a rash that **does not fade** when you press a clear glass against it (the “glass test”). It looks like tiny pinpricks that turn into purple bruises.
Other critical symptoms include:
- High fever and cold hands/feet.
- Stiff neck.
- Sensitivity to light.
- Bulging soft spot (fontanelle).
- High-pitched cry or difficult to wake.
Treatment
If you suspect meningitis or see a non-fading rash, go to the ER immediately. Bacterial meningitis needs urgent IV antibiotics. Early treatment saves lives.
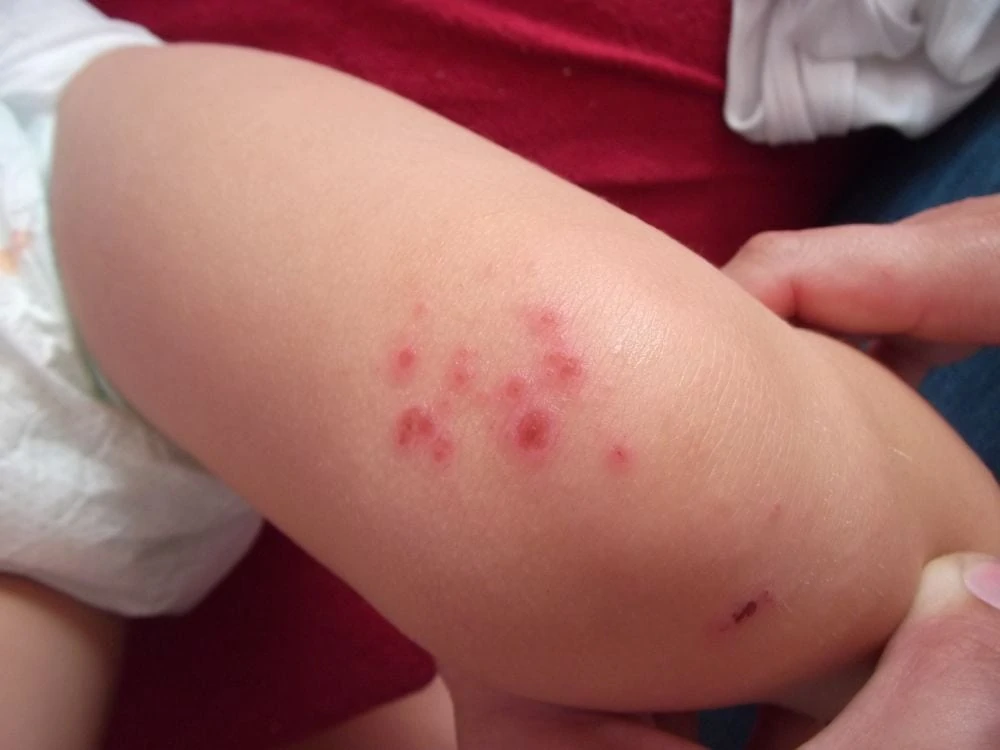
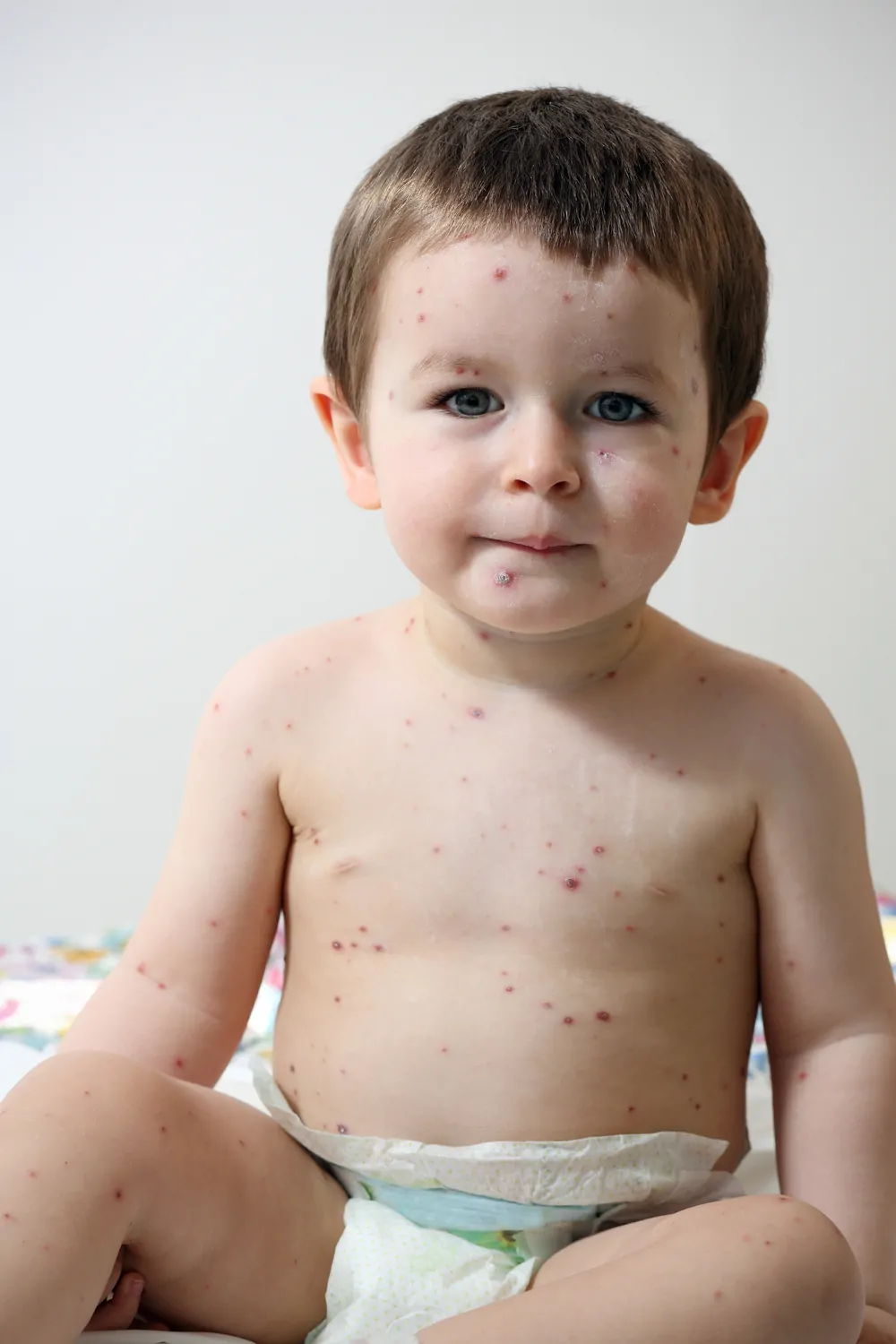
16. Chickenpox
Thanks to vaccines, chickenpox is less common now, but it still happens. It causes an itchy, blister-like rash (16).
Causes
It is caused by the varicella-zoster virus. It is highly contagious to anyone who hasn’t had the disease or the vaccine.
Symptoms
It starts with fever and fatigue. Then, red spots appear, which turn into fluid-filled blisters that eventually crust over. The rash often starts on the chest and face and spreads outward.
Treatment
Keep your baby comfortable. Oatmeal baths and calamine lotion can help the itch. Keep fingernails short to prevent infection from scratching.
Avoid aspirin and ibuprofen (unless directed by a doctor) in certain viral cases; stick to acetaminophen for fever. If your baby is under 1 year old or has a weak immune system, call your doctor.
17. Molluscum Contagiosum
Molluscum is a common viral skin infection that results in round, firm bumps. It sounds like a Harry Potter spell, but it is just a harmless skin nuisance.
Causes
It spreads through direct contact or shared objects like towels and bath toys. It loves warm, wet environments.
Symptoms
You will see small, dome-shaped bumps that are pearly or flesh-colored. They often have a tiny dimple in the center. They are usually painless but can be itchy.
Treatment
In most cases, doctors recommend leaving them alone. They will eventually go away, though it can take 6 to 18 months.
If the bumps are spreading rapidly or bothering your child, a dermatologist can remove them, but this can be painful for little ones. To prevent spreading, cover the bumps with a bandage if your child is playing with others.
When to Worry About a Rash
Babies have sensitive skin, so redness is often par for the course. However, trust your gut.
Call your pediatrician immediately if the rash:
- Is accompanied by a fever (over 100.4°F in newborns).
- Looks like purple spots or bruises.
- Does not fade when pressed (the glass test).
- Appears suddenly with lip swelling or trouble breathing (call 911).
- Is oozing, warm to the touch, or has red streaks (signs of infection).
Baby Rashes FAQs
Make a Rash Decision
Caring for your baby’s skin doesn’t have to be complicated. Stick to fragrance-free products, don’t over-bathe, and keep that diaper area dry.
Remember, most rashes look worse than they actually are. Common bumps like baby acne or heat rash are just temporary glitches as your baby’s skin adapts to the world.
However, you know your baby best. If a rash looks angry, doesn’t fade, or your little one seems sick, make that call to the pediatrician. It is always better to get peace of mind!