Is your newborn’s skin looking a little less “soft as a baby’s bottom” and a little more like a shedding reptile?
Don’t panic. Dry, peeling skin is incredibly common for new babies. After soaking in fluid for nine months, their sensitive skin needs time to adjust to the dry, harsh air of the outside world. While it usually looks worse than it feels, there are plenty of ways to help the process along.
In this article, we will cover why newborn skin peels, how to spot conditions like eczema, and the best ways to restore that famous baby softness.
Key Takeaways
- It is normal: Newborn peeling is a physiological response to losing the protective vernix caseosa after birth.
- Watch for conditions: While simple dryness is common, red patches or itchiness could signal infant eczema or ichthyosis.
- Adjust bath habits: Long, hot baths strip natural oils; switch to short, lukewarm baths to retain moisture.
- Choose products wisely: Use hypoallergenic ointments or creams and avoid scented laundry detergents to prevent irritation.
Causes of Dry Skin in Babies
Exposure to amniotic fluid is the primary reason for that flaky newborn skin. Your baby spent nine months swimming in liquid. Once they meet the dry air of the delivery room, their skin reacts by shedding its outer layer.
Interestingly, this peeling is often more intense in overdue babies. Since they stay in the womb longer, they lose their protective coating before birth, leaving their skin more vulnerable to the fluid.
Newborns that I have seen between the gestational ages of 40 to 42 weeks tend to have an excessive amount of skin peeling. By two weeks old, this peeling layer of skin sloughs off, resulting in smooth skin. Many parents ask me about using moisturizers to reduce peeling. I reassure them that moisturizers are unnecessary, and peeling skin is a normal process.
Editor's Note:
Dr. Leah Alexander, MD, FAAPFor the first 17 weeks of gestation, your baby’s skin is transparent and covered by lanugo (tiny hairs). As their skin matures, a crucial barrier develops to shield them from their watery environment.
The Role of Vernix Caseosa
Between the 17th and 20th week of pregnancy, a white, cheese-like substance called vernix caseosa covers the fetus. It is a rich blend of water, proteins, and lipids (fats) (1).
Think of vernix as a natural waterproof wetsuit. The lipids prevent the amniotic fluid from waterlogging the baby’s skin, while the water content keeps the skin hydrated.
This coating also stops the skin from peeling in utero. If the vernix stays intact until birth, the skin remains smooth. However, the vernix naturally begins to dissolve during the final weeks of pregnancy.
This explains why premature babies often arrive covered in thick white vernix, while babies born post-term usually have very little. Without that barrier, the amniotic fluid dries out their skin before they are even born, leading to immediate peeling.
Once the vernix is washed off (or absorbs completely), the shedding begins. This usually happens within the first one to three weeks. It is simply the baby’s way of discarding old skin cells to reveal a tougher, more resilient layer underneath.
Remember
Other Possible Causes of Newborn Dry Skin
While physiological shedding is the most common cause, other conditions can lead to dryness.
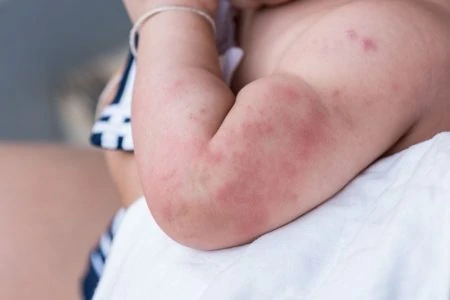
1. Infant Eczema
Eczema, or atopic dermatitis, is a chronic condition causing itchy, inflamed skin. While it is most common in children, it can appear in babies as young as 3 or 4 months old.
Unlike normal newborn peeling, eczema causes discomfort. If there is a family history of asthma or allergies, your baby has a higher risk of developing it.
Symptoms
It is easy to confuse eczema with cradle cap, but the location and texture offer clues.
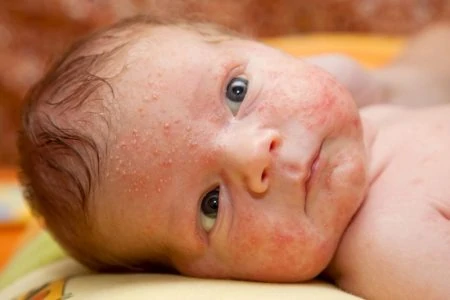
Eczema patches look thickened, red, and scaly. You might see tiny red bumps that can ooze or crust over if scratched. In babies, it typically appears on the cheeks, forehead, or scalp, and eventually spreads to the arms and legs (2).
Cradle cap, on the other hand, is usually greasy and yellow (like dandruff) rather than dry and red.
If your baby has eczema, keep their nails trimmed short. Using baby mittens prevents them from breaking the skin and causing an infection.
Watch out for these common flare-up triggers:
- Dry air: Low humidity sucks moisture from the skin.
- Irritants: Wool clothing, polyester, or scented laundry detergents.
- Heat: Sweat is a major enemy of eczema.
- Allergens: Certain foods (like dairy or soy) in the breastfeeding parent’s diet or formula.
I have seen a few infants with mild eczema that worsened when oat cereal was introduced as one of the first foods. When I asked the parent which skin products they were using, it happened to be a colloidal-oat-based moisturizer. Once the parents discontinued both the oat cereal and that particular moisturizer, the eczema resolved.
Editor's Note:
Dr. Leah Alexander, MD, FAAPWhy It Happens
Eczema is often a barrier issue. Healthy skin retains moisture and keeps germs out. In babies with eczema, the skin lacks filaggrin or ceramides (fatty cells), causing it to dry out and crack. This lets moisture escape and irritants enter.
Most babies outgrow eczema by age 2. For persistent cases, a pediatrician might prescribe a specific eczema cream. The Mayo Clinic offers excellent guidance for managing daily flare-ups.
2. Ichthyosis Vulgaris
This is a genetic disorder where the skin cannot shed dead cells properly, leading to a buildup of thick, dry scales. It is relatively rare, affecting about 1 in 250 people (3).
Symptoms
Ichthyosis usually presents around two months of age. You might notice:
- Severe dryness: Especially on the lower legs and shins.
- Scale-like appearance: The skin looks like fish scales (white, gray, or brown).
- Deep lines: Palms and soles may have extra creases.
It often spares the diaper area because the moisture there prevents the scales from forming. Treatment relies heavily on consistent use of thick moisturizers and humidifiers.
How to Treat Newborn Skin Peeling
Most peeling goes away on its own. However, you can speed up the healing process and keep your baby comfortable with these tips recommended by the AAP (4).
1. Shorten the Bath Time
Water actually dries out the skin if the exposure is too long. Limit bath time to fewer than 10 minutes.
You also do not need to bathe a newborn daily. Two to three times a week is plenty. Use lukewarm water rather than hot, as heat strips natural oils faster. Unless there was a diaper explosion, skip the soap on the torso and back; just rinse with water.
2. Lock in Moisture
Moisturize immediately after the bath. Pat your baby’s skin gently with a towel (do not rub) so it is still slightly damp, then apply your product. This seals the water into the skin.
For peeling skin, thicker is better. Ointments (like petroleum jelly) or thick creams work better than watery lotions. I used pure baby oil or coconut oil for a post-bath massage. It treated the dry skin and helped us bond.
3. Block the Cold Air
Cold air holds less moisture, which accelerates drying. When heading outdoors, cover your baby’s hands and feet. Use a loose, breathable cover over the car seat or stroller to shield their face from wind.
4. Avoid Harsh Chemicals
Newborn skin is highly permeable, meaning it absorbs whatever you put on it. Avoid products with fragrances, dyes, or sulfates.
If soap is necessary, use a mild, unscented option. Dr. Bronner’s Pure-Castile Liquid Soap is a favorite for natural-minded parents. Note that it is not tear-free, so avoid the eye area carefully.
For laundry, switch to a “free and clear” detergent. Puracy liquid detergent is plant-derived and effective. Alternatively, Molly’s Suds is a powder detergent specifically designed for sensitive skin.
5. Watch Hydration Levels
Healthy skin starts from the inside. Ensure your baby is feeding frequently. For the first six months, breast milk or formula provides all the hydration they need.
Remember
6. Use a Humidifier
Central heating and air conditioning dry out indoor air. Running a cool-mist humidifier in the nursery adds moisture back into the environment, which helps prevent itchy, dry patches overnight.
7. Try an Oatmeal Bath
Colloidal oatmeal is a superhero for irritated skin. It contains phenols and vitamin E, which reduce inflammation and soothe itching (5).
Sprinkle a packet of colloidal oatmeal into a lukewarm bath and let your baby soak for 10 minutes. It creates a milky, soothing barrier on the skin.
Take Note
When to See a Doctor
Standard newborn peeling is cosmetic and resolves on its own. However, you should consult your pediatrician if you notice signs of infection or severe allergy.
Watch for these red flags:
- Redness: Especially if it feels hot to the touch.
- Cracking: Deep fissures that bleed or ooze yellow fluid.
- Fever: Any fever in a newborn requires medical attention.
- Distress: If your baby seems extremely itchy or uncomfortable.
Baby Dry Skin and Peeling FAQs
Restore Your Newborn’s Dry Skin
Seeing your baby shed like a little lizard can be surprising, but it is a completely normal part of adjusting to life outside the womb. This is especially true for babies born past their due date who missed out on that extra vernix protection.
Keep the baths short and lukewarm, use a humidifier, and slather on the moisturizer while their skin is still damp. If you see angry red patches or signs of infection, give your pediatrician a call. Otherwise, give it a few weeks; that famously soft skin is waiting right underneath.