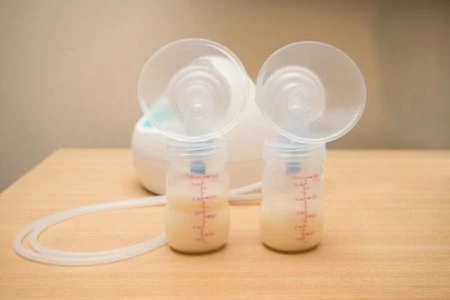
You have the implants, and now you have a baby on the way. It is completely normal to wonder if your augmentation will affect your ability to breastfeed. It is one of the most common questions plastic surgeons and lactation consultants hear.
The short answer? Yes, most women with implants can breastfeed successfully. However, the type of surgery you had, where your incisions are, and the placement of the implant can all play a role in how much milk you produce.
Let’s break down exactly how breast augmentation interacts with lactation, what challenges you might face, and how to set yourself up for success.
Key Takeaways
- Most women can breastfeed: Having implants does not automatically mean you cannot nurse, but you may face supply challenges depending on your specific surgery.
- Incision location matters: Incisions made around the nipple (periareolar) carry a higher risk of damaging milk ducts and nerves compared to under-the-breast or armpit incisions.
- Placement counts: Implants placed under the muscle usually interfere less with milk production than those placed over the muscle.
- Safety is not an issue: There is no evidence that silicone from implants leaks into breast milk or poses a risk to your baby.
Factors That Affect Milk Production
Not all breast augmentations are created equal. Several variables determine whether your milk supply will be full, partial, or minimal. Here is what you need to know:
1. Incision Location
Where the surgeon made the cut is perhaps the biggest predictor of breastfeeding success. The incision site determines how much internal “hardware” (nerves and ducts) might have been disrupted.
- Periareolar (Around the nipple): This incision goes through the areola. It carries the highest risk because it cuts through the nerves that signal your brain to make milk, as well as the ducts that carry the milk (1).
- Inframammary (Under the breast): This is the most common incision. It is generally safer for breastfeeding because it avoids the milk ducts and nerve clusters around the nipple.
- Transaxillary (Armpit) or Transumbilical (Belly button): These entry points are distant from the breast tissue, meaning the milk ducts and nerves usually remain intact.
2. Implant Placement
Where the implant sits inside your chest affects the pressure put on your milk-making glands.
- Sub-muscular (Under the muscle): The implant sits behind the pectoral muscle. This is the best scenario for breastfeeding because the muscle acts as a cushion between the implant and your glandular tissue.
- Sub-glandular (Over the muscle): The implant sits right underneath the breast tissue but on top of the muscle. The weight of the implant can exert pressure on the milk glands, potentially causing atrophy (thinning of the tissue) or reduced output over time.
3. Scarring and Capsular Contracture
Your body naturally forms a capsule of scar tissue around any foreign object, including implants.
- Hardening breasts: If this scar tissue becomes unusually hard or tight (capsular contracture), it can squeeze the milk ducts and impede flow (2).
- Pain and engorgement: Excessive internal pressure can make engorgement more painful and increase the risk of mastitis or plugged ducts because the milk cannot drain easily (3).
4. Functional Breast Tissue
Ideally, you need enough glandular tissue to produce milk.
- Pre-existing issues: Some women get implants because they have hypoplastic breasts (insufficient glandular tissue) or tubular breasts. In these cases, low milk supply is usually caused by the lack of tissue rather than the implant itself (4).
- Surgical removal: If you had a breast reduction or lift along with your implants, some milk-producing tissue might have been removed during the procedure.
5. Nipple Sensation
Breastfeeding relies on a feedback loop. When the baby sucks, nerves in the nipple send a signal to your brain to release prolactin (makes milk) and oxytocin (flows milk).
- Numbness: If you have lost sensation in your nipples post-surgery, that “order” might not get sent to the brain efficiently (5).
- Hypersensitivity: Conversely, some women find their nipples are painfully sensitive after surgery, making the sensation of breastfeeding difficult.
Does The Surgical Technique Matter?
Absolutely. We touched on incisions briefly, but let’s look closer at how specific techniques correlate with breastfeeding success rates.
1. Inframammary (The Fold Incision)
This is widely considered the “breastfeeding-friendly” approach. The surgeon cuts along the crease where the breast meets the chest wall. Because the entry point is low, they rarely need to cut through the breast tissue itself to place the implant. Nerves and ducts usually remain untouched.
2. Trans-Axillary (The Armpit Incision)
Surgeons use an endoscope (camera) to slide the implant in through the armpit. Like the fold incision, this avoids direct trauma to the breast tissue. The path goes behind the breast, leaving the nipple-areola complex alone. This method generally has a very good prognosis for nursing.
3. Periareolar (The Nipple Incision)
This technique hides the scar well along the border of the areola, but it is the most disruptive to breastfeeding. To get the implant in, the surgeon must cut through the breast tissue.
Studies suggest that women with this incision type are significantly more likely to struggle with milk supply compared to other methods (6). If you are planning surgery and know you want to breastfeed later, discuss this risk with your surgeon.
4. Transumbilical (The Belly Button Incision)
This less common method involves tunneling up from the navel. While it avoids a scar on the breast, the tunneling process can sometimes cause internal trauma. Generally, though, it is considered less risky for milk production than the periareolar cut.
Can Damaged Nerves Heal?
Here is some good news: nerves can regenerate. If it has been several years since your surgery, your body may have performed its own repairs. This process is called recanalization.
Furthermore, pregnancy itself is a massive booster for breast tissue. The hormonal surges causing your breasts to grow during pregnancy are actually stimulating the growth of new glandular tissue and ducts (7).
This means even if you had some damage, the remaining healthy tissue can hypertrophy (grow larger) to compensate. Many moms find they produce more milk with their second or third baby than they did with their first because that tissue continues to develop with each pregnancy.
Tips for Success: Nursing with Implants
You are cleared to breastfeed, but you might need a game plan to maximize your supply.
- Nurse frequently: The more milk you remove, the more you make. Aim for 8 to 12 feedings every 24 hours in the newborn stage.
- Skin-to-skin contact: This boosts oxytocin, which helps with milk let-down and bonding.
- Breast compressions: If you have implants, you might have to work a little harder to empty the breast. Gently squeezing the breast while the baby sucks helps push milk forward past any pressure points caused by the implant.
- Work with a pro: Hire an IBCLC (International Board Certified Lactation Consultant). They can help you with latching deeper, which is often tricky if breasts are firm from implants.
- Consider pumping: Adding a session with a hospital-grade electric breast pump after nursing can help stimulate more production.
- Monitor weight gain: The best way to know if baby is getting enough is by tracking wet diapers and weight gain. If supply is low, you can supplement with formula or donor milk while still nursing for comfort and bonding.
Is Silicone Safe for the Baby?
This is a huge worry for many moms, but the science is reassuring. Whether you have saline (saltwater) or silicone gel implants, the outer shell is made of silicone.
Silicone is highly stable and heat resistant. It is used in medical tubing, IV catheters, and even infant bottle nipples.
Multiple studies, including reviews by the Institute of Medicine, have found no evidence that silicone breast implants cause systemic disease or toxicity in nursing infants.
- Silicone is everywhere: Interestingly, cow’s milk and store-bought infant formula actually contain higher levels of silicon (the element) than the breast milk of women with implants (8).
- No increased defects: The FDA and CDC state there is no association between breast implants and birth defects in children born to women with implants (9).
Rest assured, your milk is considered safe for your baby.
FAQs
Fed is Best
Breastfeeding with implants is absolutely possible, and many mothers do it successfully for months or years.
However, it is important to be realistic. The location of your incision and the placement of your implant can create hurdles for your supply. If you find that you need to supplement with formula, do not beat yourself up.
Your baby needs a happy, healthy mom more than they need exclusive breast milk. Whether you are exclusively nursing, combo-feeding, or exclusively pumping, you are doing a great job.