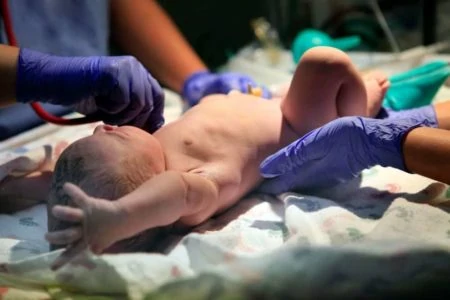
It is vital to understand that while often peaceful, home birth is not without risks. The key to a safe delivery is education and preparation. We will walk you through the real pros, cons, and safety statistics so you can decide if a home birth is the right path for your family.
The Pros and Cons of Home Birth
Advantages of Home Birth
- Comfort of familiar surroundings: You know every corner of your home. That familiarity helps you relax, which can actually help labor progress when you feel scared or in pain.
- Control over your environment: You set the rules. You can dim the lights, burn your favorite candles, or play a specific playlist without asking permission.
- Unlimited visitors and family support: There are no visiting hours in your living room. Your mom, best friend, or older children can be there as much or as little as you want.
- Sleep in your own bed: After the hard work is done, you don’t have to listen to hospital beeps or nurses coming in every hour. You get to curl up in your own sheets.
- Freedom to eat and drink: Hospitals often restrict you to ice chips. At home, you can eat comfortably to keep your energy up, provided you can keep the food down.
- More autonomy over birthing positions: You can walk, squat, use a birth stool, or labor in a shower whenever you want. You aren’t confined to a bed or hooked up to continuous monitoring cables unless necessary.
- Potential cost savings: A home birth can be significantly cheaper than a hospital birth, especially if you have a high-deductible insurance plan and an uncomplicated delivery.
- Holistic postpartum care: Midwives often provide extensive follow-up care in your home. This includes lactation support and checking on your recovery without you having to drive to a clinic a few days after birth.
Risks of Home Birth
- Limited emergency interventions: This is the biggest factor. If you need an emergency C-section or sophisticated neonatal resuscitation, you have to wait for transport. Hospitals have these tools seconds away.
- Insurance coverage issues: Some insurance providers do not cover home births, or they offer very limited reimbursement for out-of-network midwives. You might have to pay out of pocket.
- No pharmaceutical pain relief: There is no option for an epidural at home. You must rely entirely on natural pain management techniques like breathing, water, and movement.
- Hospital transfer risks: If complications arise, you will need to be transported to a hospital. This transition can be stressful and delays critical care in true emergencies.
- Midwife qualifications vary: Not all midwives have the same level of training. It is crucial to vet your provider to ensure they are equipped to handle complications.
- Administrative responsibilities: You are often responsible for the paperwork. This includes filing the birth certificate and applying for a social security number, which the hospital usually handles for you.

Home Birth vs. Hospital Birth Statistics
Emotions run high when discussing birth locations, so it helps to look at the hard data. Understanding the numbers can help you weigh the relative risks against the benefits.
U.S. Home Births vs. Hospital Births
Home births are still a minority choice in the U.S., representing roughly 1.26 percent of all births in 2021 (1). While the numbers are rising, the vast majority of women still choose hospital settings.
Neonatal Mortality Rates
This is the statistic most parents worry about. The data shows that the absolute risk of infant death is low in both settings, but it is statistically higher at home.
For hospital births attended by a certified nurse-midwife (CNM), the neonatal mortality rate was roughly 3.2 deaths per 10,000 births. For home births attended by a CNM, that number rose to roughly 10 per 10,000 (2).
The risk increases significantly if the birth is unattended or attended by an uncertified provider. This highlights the importance of choosing a Certified Nurse-Midwife (CNM) or a Certified Professional Midwife (CPM) who carries proper accreditation.
Keep It In Perspective
Likelihood of Medical Interventions
While safety risks are slightly higher at home, the risk of unnecessary medical intervention is drastically lower. Moms who choose home birth are far less likely to undergo major surgery or instrumental deliveries.
Here is how the intervention rates compare (3):
- Inducing labor: Occurs in only about 4.8 percent of out-of-hospital births, compared to 30.4 percent in hospitals.
- Cesarean delivery: The C-section rate is roughly 5.3 percent for planned out-of-hospital births, compared to a staggering 24.7 percent (or higher) in hospitals.
- Operative vaginal delivery: Forceps or vacuum use happens in about 1 percent of home births, versus 3.5 percent in hospitals.
- Episiotomy: You are much less likely to receive a surgical cut to the perineum at home.
Hospital Transfer Rate
Sometimes, a plan needs to change. The “transfer rate” refers to how often a planned home birth ends up moving to the hospital.
For first-time moms, the transfer rate is high, ranging from 23 percent to 45 percent. This is often due to labor failing to progress or the mother becoming exhausted. For women who have given birth before, the transfer rate drops significantly to between 5 percent and 12 percent (4).
Home Birth After Cesarean (HBAC)
If you had a C-section previously, a home birth is considered higher risk. This is known as a trial of labor after Cesarean (TOLAC). Because of the slight risk of uterine rupture, many providers recommend being near an operating room. However, some midwives will attend HBACs if you have had a successful vaginal birth since your C-section.
I firmly believe that every woman should be offered the opportunity for a Vaginal Birth after Cesarean (VBAC). Unfortunately, many hospitals do not provide that option.
The concern with giving birth at home is that women who have had uterine surgery have a slightly increased risk of uterine rupture, but this risk is less than 1 per 100 women (5). If your home is a far distance from the hospital or your birth attendant does not have a good relationship with a back-up physician, you and your baby’s life could be in jeopardy. It’s important to know your comfort level and to be aware of the risks and benefits.
Editor's Note:
Caitlin Goodwin, MSN, RN, CNMHome Birth FAQs
You’re In Charge
Your body and your baby mean you get to make the call. Whether you choose the living room or the delivery ward, the most important thing is that you feel safe and supported.
Remember to be your own advocate. If you choose a home birth, ensure you have a qualified team and a backup plan. If things don’t go exactly as you envisioned, knowing you made informed choices will give you peace of mind.
Find a birth professional who is well-trained in emergencies and will respect you and your family’s wishes. Unassisted birthing can have some pretty significant risks. I believe in respecting a patient’s autonomy, but please do not make this choice lightly.
Editor's Note:
Caitlin Goodwin, MSN, RN, CNMWhile most home births are safe, they do carry slightly increased risks for the baby. Make sure you screen carefully for high-risk conditions and keep an open mind about transferring if your midwife suggests it.