When it comes to giving birth, few topics spark as much debate as pain management. Should you go for the “natural” unmedicated route or opt for the relief of an epidural?
There is no single right answer. In this guide, we will break down exactly how an epidural works, why some moms prefer unmedicated birth, and the risks and rewards of both options so you can make the best choice for your body.
Key Takeaways
- Epidural: A regional anesthesia injected into the spine to block nerve signals, effectively numbing the lower body and reducing labor pain.
- Natural Birth: An unmedicated vaginal delivery where the mother manages pain through breathing, movement, and mindset rather than drugs.
- The Trade-off: Epidurals offer immense relief and rest but limit movement; unmedicated birth offers physical freedom but requires enduring intense sensation.
- Your Choice: The “right” decision depends on your pain tolerance, medical history, and how you want to experience the birth process.
Let’s start with the most popular form of pain control in delivery rooms: the epidural. According to the CDC, over 60 percent of women choose an epidural during labor.
So, why is it the go-to choice for so many moms? And is it right for you?
What Is an Epidural?
An epidural is a medical procedure where an anesthetic is injected into the epidural space of the spine. This blocks pain signals from traveling from your lower body to your brain (1). The epidural space is the area between the protective covering of the spinal cord (dura mater) and the spinal column itself (2).
Once the medication kicks in, it numbs the nerves. You might still feel pressure, but the sharp pain of contractions fades away. Because labor can last a long time, a thin catheter (tube) is usually threaded into your back to deliver continuous relief until the baby arrives.
The Benefits of an Epidural
The primary benefit is obvious: pain relief. By blocking nerve receptors, an epidural significantly decreases the intensity of contractions. This allows you to rest, relax, and stay present during the delivery.
However, the benefits go beyond just numbing the pain. Once you get an epidural, you may also experience a decrease in (3):
- Fatigue (allowing you to sleep before pushing).
- Irritability and stress hormones.
- Panic or anxiety.
- High blood pressure spikes caused by pain.
The Risks of an Epidural
While epidurals are generally safe, they are a medical intervention, and they come with risks. Knowing these ahead of time can help you prepare.
Common risks include:
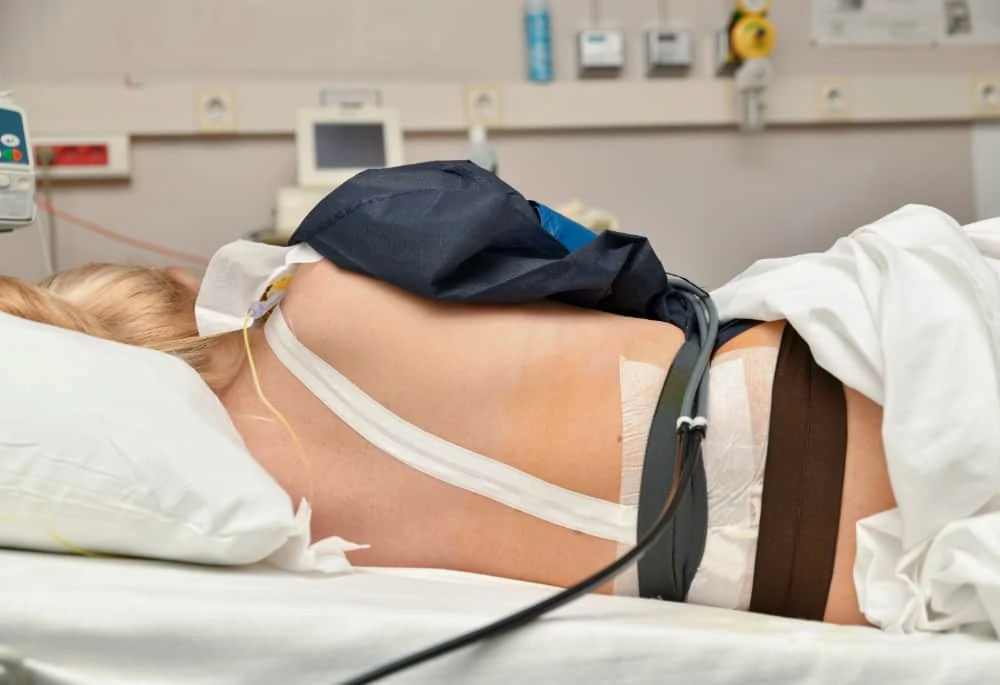
- Low Blood Pressure: This is the most common side effect. The medication can cause your blood pressure to drop, which may lower the baby’s heart rate. Your care team will monitor this closely and give you fluids to stabilize it.
- Fever: Women with epidurals are more likely to develop a fever during labor. This can sometimes lead to the baby undergoing tests for infection after birth, even if they are healthy (4).
- Prolonged Labor: Studies show epidurals may lengthen the second stage of labor (pushing) because you cannot feel the contractions as effectively.
- Instrumental Delivery: Because it is harder to feel where and when to push, there is a slightly higher chance of needing assistance from forceps or a vacuum extractor.
- Back Pain: You might feel soreness at the injection site for a few days. However, long-term chronic back pain is typically not caused by epidurals, despite common myths (5).
- Headaches: In rare cases (about 1 percent), the needle punctures the dura (the spinal covering), causing a “spinal headache.” This is treatable but can be painful and linger for a few days.
Regarding C-sections: Historically, people feared epidurals caused C-sections. However, massive studies (like those from the Cochrane Library) have largely debunked this. Having an epidural does not significantly increase your risk of needing a C-section (6).
Trust your instincts. If something feels off during the procedure or labor, speak up immediately.
Side Effects of an Epidural
Aside from the medical risks, you might experience some annoying but temporary physical side effects:
- Itching: Common if opioids are used in the epidural mix.
- Shivering: Many women experience uncontrollable shaking or shivering.
- Nausea or vomiting.
- Difficulty urinating (a catheter is often placed to help empty the bladder).
- Numbness or heavy legs, making movement difficult.
These effects generally wear off within a few hours of the medication stopping.
What Is a Natural Birth?
“Natural birth” is a common term for an unmedicated vaginal delivery. This means giving birth without pain medication, such as epidurals or opioids. Instead, the mother relies on breathing techniques, movement, water, massage, and mindset to cope with labor.
The Benefits of a Natural Birth
Why choose the unmedicated route? For many, it is about feeling connected to the process and maintaining bodily autonomy.
Here are the potential advantages (7):
- Control & Awareness: You remain fully alert and in touch with every sensation. You know exactly when to push and can work instinctively with your body.
- Freedom of Movement: Without numbness or IV poles, you can walk, squat, use a birthing ball, or change positions freely. Gravity is a great tool for speeding up labor.
- Faster Recovery: Without heavy anesthesia leaving your system, many moms feel alert and ready to walk shortly after delivery. You also avoid the common side effects of epidurals like itching or grogginess.
- Pushing Efficiency: Because you can feel the “ferguson reflex” (the body’s urge to push), unmedicated pushing stages are often shorter and more effective.
- Setting Flexibility: You aren’t tied to a hospital bed. This opens the door for home births or birthing centers if you have a low-risk pregnancy.
The Disadvantages of a Natural Birth
The main drawback? The pain. Labor is intense, and without medication, you will feel the full force of every contraction. This can be exhausting and, for some, traumatic if they are not mentally prepared or supported.
Additionally, if you plan a birth outside of a hospital (like at home), you assume the risk of transport time if an emergency arises. If complications occur, such as the baby showing distress, you may need to transfer to a hospital for medical interventions (8).
If you choose this route, hiring a doula or having a strong support partner is highly recommended to help you cope with the intensity.
Epidural vs. Natural Birth: How to Choose
Choosing between an epidural and an unmedicated birth is personal. There is no award for suffering, and there is no shame in pain relief.
Ask yourself these questions to help guide your decision:
- Is my pregnancy high-risk or low-risk? (High-risk often requires hospital monitoring).
- What is my personal pain tolerance?
- Do I want to be able to walk around during labor?
- Does the idea of a needle in my spine cause me anxiety?
- Do I have access to a doula to help with pain management techniques?
- Does my hospital have 24/7 anesthesia support?
- How do I typically handle stress and exhaustion?
- If I plan to go natural, am I open to changing my mind if labor is prolonged?
Remember, you can write a birth plan, but birth is unpredictable. Being flexible is the best way to avoid disappointment.
Some hospitals have no anesthesiologist and no ability to get an epidural. There are other things that can be done that bridge the gap between an epidural and natural birth that you can talk to your doctor or midwife about if you want something other than an epidural or natural birth.
Editor's Note:
Caitlin Goodwin, MSN, RN, CNMOther Birth Options
It isn’t just black and white. If you want to avoid an epidural but need some help, there are middle-ground options (9).
- Nitrous Oxide (Laughing Gas): Inhaled through a mask during contractions. It doesn’t remove pain completely but creates a sense of detachment and relaxation. It clears your system instantly.
- IV Pain Medication: Opioids (like Stadol or Fentanyl) can be given through an IV. They “take the edge off” and help you rest, though they can make you and the baby sleepy.
- Sterile Water Injections: Tiny amounts of sterile water are injected under the skin of the lower back. It stings briefly but provides excellent relief for back labor.
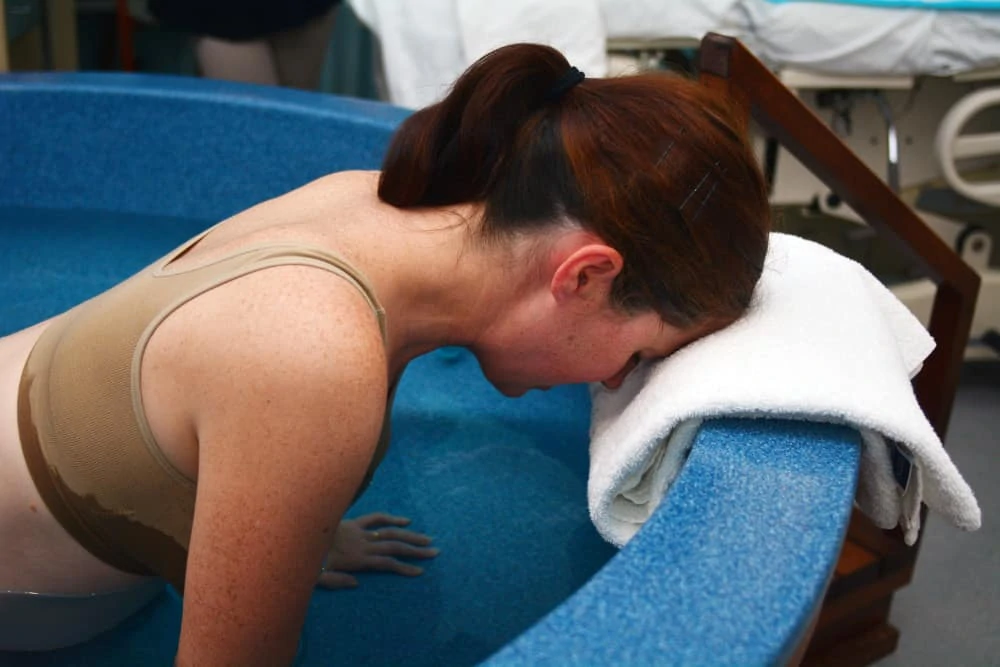
- Hydrotherapy: Laboring in a tub or shower. The warm water acts as a natural pain reliever and muscle relaxer.
- TENS Unit: A device that sends small electrical pulses to pads on your back, distracting the nerves from pain signals.